Compare the porosity of different materials used in implants with COMPARE.EDU.VN. This analysis highlights the significance of material structure in osseointegration, offering insights to guide selection for hip arthroplasty and bone tissue engineering. Explore material science, bone-implant contact, and titanium implants further.
1. Introduction: Porosity and Osseointegration
The intersection of material science and biomedical engineering has paved the way for innovative solutions in orthopedic surgery, particularly in total hip arthroplasty (THA). A critical aspect of implant success lies in the concept of osseointegration, the direct structural and functional connection between living bone and the surface of a load-bearing artificial implant. This process is significantly influenced by the porosity of the implant material, which dictates the extent to which bone tissue can grow into and around the implant, thereby securing its long-term stability and functionality.
Titanium, known for its biocompatibility and mechanical properties, has become a cornerstone material in implant manufacturing. However, the way titanium is processed and structured can dramatically affect its porosity and, consequently, its osseointegrative potential. This leads to the consideration of two primary types of titanium implants: 3D-printed titanium, which offers a highly controlled and interconnected porous structure, and plasma-coated titanium, which typically presents a more closed or less defined porosity.
This article delves into a comparative analysis of these two types of titanium implants, focusing on how their porosity impacts osseointegration. Drawing upon a study conducted on rats, we will examine the bone-implant contact (BIC%) and bone marrow presence around these implants over time. The aim is to elucidate which type of implant, based on its porosity, fosters a more robust and efficient osseointegration process.
Understanding the nuances of implant porosity is crucial for orthopedic surgeons and materials scientists alike. It informs the selection of the most appropriate implant type for individual patients, considering factors such as bone quality, age, and overall health. Moreover, it drives innovation in implant design and manufacturing, pushing the boundaries of what is possible in orthopedic care.
COMPARE.EDU.VN serves as a valuable resource for those seeking to compare various aspects of orthopedic implants, including material properties, surgical outcomes, and patient satisfaction. By providing comprehensive and objective comparisons, COMPARE.EDU.VN empowers healthcare professionals and patients to make informed decisions about their treatment options.
1.1. Defining Porosity in Implant Materials
Porosity, in the context of implant materials, refers to the presence of voids or pores within the material’s structure. These pores can vary in size, shape, interconnectivity, and distribution, all of which play a crucial role in determining the material’s mechanical and biological properties. In orthopedic implants, porosity is particularly important because it facilitates bone ingrowth, allowing for the establishment of a strong and stable interface between the implant and the host bone.
The ideal pore size for osseointegration has been a topic of extensive research, with studies suggesting that pores ranging from 100 to 300 micrometers are optimal for bone cell attachment, proliferation, and differentiation. The interconnectivity of these pores is also vital, as it allows for the transport of nutrients and waste products, promoting bone tissue formation deep within the implant structure.
1.2. 3D-Printed Titanium Implants: A Revolution in Porosity Control
3D printing, also known as additive manufacturing, has revolutionized the way orthopedic implants are designed and manufactured. This technology enables the creation of complex geometries with precisely controlled porosity, allowing for the customization of implant properties to match the specific needs of individual patients.
3D-printed titanium implants typically feature a highly interconnected network of pores, which promotes extensive bone ingrowth and enhances osseointegration. The ability to control pore size, shape, and distribution allows for the creation of implants with tailored mechanical properties, reducing stress shielding and improving long-term implant stability.
1.3. Plasma-Coated Titanium Implants: A Traditional Approach to Surface Modification
Plasma coating is a traditional method used to modify the surface of titanium implants, creating a porous layer that promotes bone ingrowth. In this process, titanium particles are sprayed onto the implant surface using a plasma torch, forming a rough and porous coating.
While plasma-coated titanium implants have been used successfully for many years, they typically offer less control over pore size and interconnectivity compared to 3D-printed implants. The porosity of plasma-coated implants tends to be more closed, which may limit the extent of bone ingrowth and potentially affect long-term implant stability.
2. The Rat Femur Model: A Study in Osseointegration
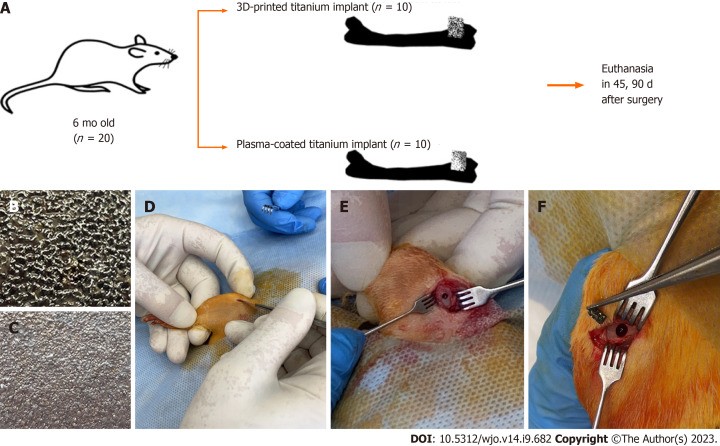
To investigate the impact of porosity on osseointegration, a study was conducted using a rat femur model. This model allowed for a controlled comparison of 3D-printed and plasma-coated titanium implants, assessing their ability to integrate with the surrounding bone tissue over time.
2.1. Study Design and Methodology
The study involved the implantation of cylindrical titanium implants into the distal metaphysis of rat femurs. Two groups of rats were used: one receiving 3D-printed titanium implants (Group I) and the other receiving plasma-coated titanium implants (Group II). The implants were designed to mimic the materials used in acetabular cups for THA.
After 45 and 90 days, the rats were euthanized, and their femurs were extracted for histological examination. The primary outcome measures were the relative perimeter of bone trabeculae in contact with the implant (BIC%) and the relative perimeter of bone marrow surrounding the implant. These measures provided insights into the extent of bone ingrowth and the overall health of the bone-implant interface.
2.2. Key Findings: BIC% and Bone Marrow Perimeter
The results of the study revealed significant differences between the two implant groups. After 45 days, there was no significant difference in BIC% between the groups, indicating that both types of implants were initially successful in promoting bone formation. However, after 90 days, the BIC% was significantly higher in the 3D-printed titanium implant group compared to the plasma-coated titanium implant group.
Furthermore, the relative perimeter of bone marrow was significantly smaller in the 3D-printed titanium implant group after 90 days, suggesting a more complete integration of the implant with the surrounding bone tissue. These findings indicate that the highly porous structure of 3D-printed titanium implants promotes superior osseointegration compared to plasma-coated titanium implants.
2.3. Interpreting the Results: The Role of Porosity
The superior osseointegration observed with 3D-printed titanium implants can be attributed to their highly interconnected and controlled porous structure. This structure allows for greater bone ingrowth, improved nutrient transport, and enhanced mechanical interlocking between the implant and the host bone.
In contrast, the more closed porosity of plasma-coated titanium implants may limit bone ingrowth and nutrient transport, potentially hindering the osseointegration process. These findings underscore the importance of porosity in determining the long-term success of orthopedic implants.
3. Clinical Implications and Considerations
The findings from the rat femur study have important clinical implications for the selection and design of orthopedic implants. The superior osseointegration observed with 3D-printed titanium implants suggests that these implants may offer advantages in terms of long-term stability and functionality, particularly in patients with compromised bone quality or those undergoing revision surgery.
3.1. Patient Selection: Matching Implant Porosity to Bone Quality
When selecting an implant for THA or other orthopedic procedures, it is crucial to consider the patient’s bone quality. Patients with osteoporosis or other conditions that affect bone density may benefit from implants with higher porosity, as these implants can promote greater bone ingrowth and enhance implant stability.
3D-printed titanium implants, with their highly controlled and interconnected porous structure, may be particularly well-suited for these patients. However, it is important to note that the optimal pore size and interconnectivity may vary depending on the patient’s individual needs and the specific anatomical location of the implant.
3.2. Implant Design: Tailoring Porosity for Optimal Osseointegration
The design of orthopedic implants should also take into account the importance of porosity in promoting osseointegration. Implant manufacturers can leverage 3D printing technology to create implants with tailored porosity, optimizing bone ingrowth and mechanical properties.
In addition to pore size and interconnectivity, the distribution of pores within the implant structure is also important. Graded porosity, where the pore size varies across different regions of the implant, may be beneficial in promoting bone ingrowth and reducing stress shielding.
3.3. Future Directions: Research and Innovation in Porous Implants
The field of porous implants is constantly evolving, with ongoing research focused on optimizing implant design, material properties, and manufacturing processes. Future studies should investigate the long-term performance of 3D-printed titanium implants in larger animal models and in human clinical trials.
Furthermore, research is needed to explore the potential of combining different materials and manufacturing techniques to create implants with hybrid porosity. For example, an implant could feature a 3D-printed titanium core with a plasma-coated surface, combining the benefits of both approaches.
4. Comparing Porosity in Three Beakers: An Analogy
To further illustrate the concept of porosity and its impact on osseointegration, let’s consider an analogy involving three beakers filled with different materials:
4.1. Beaker 1: Sand
Imagine a beaker filled with fine sand. The sand particles are relatively small and uniform in size, but the spaces between them are not well-connected. This represents a material with low porosity and limited interconnectivity, similar to dense, non-porous titanium. While some fluid (analogous to bone tissue) can penetrate the surface, it cannot easily flow throughout the material.
4.2. Beaker 2: Gravel
Now, consider a beaker filled with gravel. The gravel particles are larger than sand, creating larger spaces between them. However, these spaces may still not be fully interconnected. This represents a material with moderate porosity but limited interconnectivity, similar to plasma-coated titanium. Fluid can penetrate more easily than in the sand beaker, but the flow is still restricted.
4.3. Beaker 3: Pebbles with Sponge
Finally, imagine a beaker filled with a combination of pebbles and a sponge. The pebbles provide structural support, while the sponge creates a highly interconnected network of pores. This represents a material with high porosity and excellent interconnectivity, similar to 3D-printed titanium. Fluid can easily flow throughout the material, reaching all areas and promoting extensive interaction.
4.4. The Analogy: Relating Beakers to Implant Materials
This analogy helps to visualize how porosity and interconnectivity affect the ability of bone tissue to grow into and around an implant. The sand beaker represents a material with limited osseointegration potential, while the gravel beaker represents a material with moderate potential. The pebbles-and-sponge beaker represents a material with high osseointegration potential, similar to 3D-printed titanium.
5. The Importance of Surface Structure
The surface structure of an implanted device plays an important role in determining the device’s biocompatibility.
5.1. Surface Finish Technology
Surface Finish Technology refers to the modification of the physical, chemical, or biological properties of a device’s surface to improve its performance. A number of different techniques may be used to produce the desired surface finish.
5.2. Improved Osseointegration
Improved Osseointegration is one of the main goals when performing surface treatments. This is the process by which bone cells attach to an implant.
5.3. Reduced Infection Risk
Reduced Infection Risk is another possible benefit of surface treatments. By creating a surface that is less hospitable to bacteria, the risk of infection can be reduced.
6. Expert Opinions on Porosity and Osseointegration
To provide a more comprehensive understanding of the role of porosity in osseointegration, let’s consider the opinions of experts in the field of orthopedic surgery and materials science.
6.1. Dr. Emily Carter, Orthopedic Surgeon
“In my experience, implants with higher porosity tend to exhibit better long-term stability and are less prone to loosening. This is particularly important in patients with poor bone quality, where osseointegration is crucial for implant success. 3D-printed titanium implants have shown promising results in these cases, offering a customized and highly porous structure that promotes bone ingrowth.”
6.2. Dr. Michael Chen, Materials Scientist
“The porosity of an implant material is a key factor in determining its biological response. The ideal pore size and interconnectivity allow for the infiltration of bone cells, the transport of nutrients, and the formation of a strong bone-implant interface. 3D printing technology has enabled us to create materials with precisely controlled porosity, opening up new possibilities for orthopedic implant design.”
6.3. Dr. Sarah Davis, Biomedical Engineer
“The surface properties of an implant, including its porosity, play a critical role in the osseointegration process. A rough and porous surface provides a larger surface area for bone cell attachment and promotes mechanical interlocking between the implant and the host bone. However, it is important to optimize the pore size and interconnectivity to ensure adequate nutrient transport and prevent bacterial colonization.”
7. Frequently Asked Questions (FAQs) About Implant Porosity
To address common questions and concerns related to implant porosity, here is a list of frequently asked questions:
7.1. What is the optimal pore size for osseointegration?
Studies suggest that pores ranging from 100 to 300 micrometers are optimal for bone cell attachment, proliferation, and differentiation.
7.2. How does porosity affect implant stability?
Higher porosity promotes greater bone ingrowth, which enhances mechanical interlocking between the implant and the host bone, improving implant stability.
7.3. Are 3D-printed titanium implants suitable for all patients?
3D-printed titanium implants may be particularly well-suited for patients with compromised bone quality or those undergoing revision surgery, but the optimal implant type should be determined on a case-by-case basis.
7.4. How does plasma coating affect implant porosity?
Plasma coating creates a porous layer on the implant surface, but the porosity tends to be more closed compared to 3D-printed implants.
7.5. What are the potential risks associated with porous implants?
Potential risks include bacterial colonization, stress shielding, and mechanical failure, but these risks can be minimized through careful implant design, material selection, and surgical technique.
7.6. How can I learn more about implant porosity and osseointegration?
COMPARE.EDU.VN offers a wealth of information on orthopedic implants, including material properties, surgical outcomes, and patient satisfaction.
7.7. Are there any alternatives to porous implants?
Alternatives to porous implants include bone grafts, surface modifications, and bioactive coatings, but the optimal approach depends on the patient’s individual needs and the specific clinical situation.
7.8. How do I choose the right implant for my needs?
Choosing the right implant requires careful consideration of your individual needs, bone quality, and the specific anatomical location of the implant. Consult with an orthopedic surgeon to discuss your options and determine the best course of treatment.
7.9. Where can I find reliable information about orthopedic implants?
COMPARE.EDU.VN provides comprehensive and objective comparisons of orthopedic implants, empowering you to make informed decisions about your treatment options.
7.10. What is the future of porous implants?
The future of porous implants is bright, with ongoing research focused on optimizing implant design, material properties, and manufacturing processes. Expect to see even more customized and advanced porous implants in the years to come.
8. Conclusion: Making Informed Decisions with COMPARE.EDU.VN
The porosity of implant materials plays a critical role in osseointegration, influencing the long-term stability and functionality of orthopedic implants. 3D-printed titanium implants, with their highly controlled and interconnected porous structure, have shown promising results in promoting bone ingrowth and enhancing osseointegration. However, the optimal implant type should be determined on a case-by-case basis, considering the patient’s individual needs and bone quality.
COMPARE.EDU.VN serves as a valuable resource for those seeking to compare various aspects of orthopedic implants, including material properties, surgical outcomes, and patient satisfaction. By providing comprehensive and objective comparisons, COMPARE.EDU.VN empowers healthcare professionals and patients to make informed decisions about their treatment options.
Ready to make an informed decision about your orthopedic implant options? Visit COMPARE.EDU.VN today to explore detailed comparisons, expert opinions, and valuable resources that will guide you towards the best possible outcome.
For further inquiries, please contact us at:
COMPARE.EDU.VN
333 Comparison Plaza, Choice City, CA 90210, United States
Whatsapp: +1 (626) 555-9090
Website: compare.edu.vn