The American College of Surgeons National Surgical Quality Improvement Program (ACS NSQIP) surgical risk calculator is a valuable tool for predicting postoperative outcomes. But how accurate are its predictions for complex procedures like pancreaticoduodenectomy (PD)? This study examines the calculator’s performance in a cohort of PD patients, comparing predicted and observed results. We delve into whether incorporating specific diagnoses, using ICD-9 codes, enhances the calculator’s predictive capabilities.
Keywords: NSQIP, universal risk calculator, pancreaticoduodenectomy, predicted results, observed results, surgical outcomes, risk prediction
Introduction: Predicting Outcomes in Pancreaticoduodenectomy
The ACS NSQIP surgical risk calculator provides estimated probabilities of various postoperative complications. This information is crucial for informed consent and shared decision-making between surgeons and patients. While the calculator has been validated across diverse surgical procedures, its accuracy in predicting outcomes for complex operations like PD warrants further investigation. This study aims to address this gap by comparing the calculator’s predicted results with observed outcomes in a cohort of PD patients.
Methods: Comparing Predicted and Observed Outcomes
A random sample of 400 PD patients from the NSQIP database (2005-2012) was analyzed. Patients were grouped based on ICD-9 diagnosis: benign neoplasms, pancreatic cancer, ampullary carcinoma, and chronic pancreatitis. Preoperative variables were entered into the NSQIP universal risk calculator to generate predicted probabilities for various postoperative outcomes. The Brier Score (BS) was used to compare predicted probabilities with observed outcomes. A BS of 0 indicates perfect prediction, while a BS of 1 represents the poorest prediction. The calculated BS was then compared to a null model BS to assess the calculator’s accuracy.
Results: Analyzing the Accuracy of the Risk Calculator
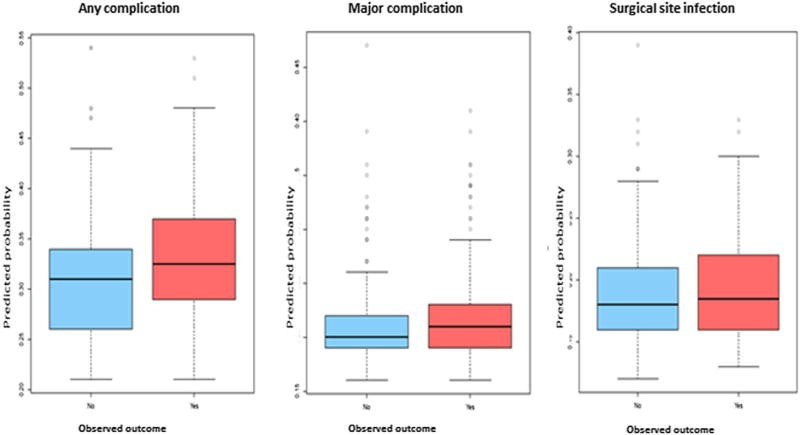
The overall BS for the entire cohort was generally low, suggesting good predictive ability. However, the BS for “any complication” and “major complication” was higher (0.23 and 0.22, respectively), indicating less accurate prediction for these broader categories.
When stratified by ICD-9 diagnosis, patients with ampullary carcinoma exhibited the highest incidence of complications (47%). The BS for any complication and major complication was also higher in this subgroup (0.27 and 0.26, respectively), suggesting a potential influence of diagnosis on predictive accuracy. This finding was further supported by the comparison with the null model BS.
Discussion: The Role of Diagnosis in Risk Prediction
This study highlights the importance of considering specific diagnoses when assessing surgical risk in PD. The observed variation in predictive accuracy across different ICD-9 subgroups suggests that incorporating diagnosis-specific variables could enhance the calculator’s performance. While the NSQIP calculator provides a valuable tool for risk stratification, its limitations in capturing the nuances of specific disease processes underscore the need for ongoing refinement and the potential incorporation of disease-specific variables.
Conclusion: Refining Risk Prediction for Pancreaticoduodenectomy
The ACS NSQIP surgical risk calculator demonstrates reasonable accuracy in predicting postoperative outcomes for PD. However, the study revealed that the calculator’s predictive capabilities vary depending on the specific diagnosis. Incorporating ICD-9 codes and disease-specific variables into future iterations of the calculator could improve risk estimation and ultimately enhance preoperative counseling and shared decision-making. This refinement would allow for a more personalized risk assessment, leading to better-informed choices for both surgeons and patients undergoing PD.